The specialty of anesthesiology has evolved dramatically since the first public demonstration of ether use in the 19th century. Originally, the emphasis was completely on providing surgical anesthesia. As surgical procedures became more diverse and complex, other associated skills were developed. For example, airway management, including endotracheal intubation, was required to provide controlled ventilation to patients who had respiratory depression and paralysis from neuromuscular blocking drugs. These practices required the development of a “recovery room,” which was later termed a postoperative or postanesthesia care unit (PACU). The skills that anesthesiologists used in the recovery room evolved and progressed into intensive care units (ICUs) and the specialty of critical care medicine. The development of regional anesthesia created opportunities for treatment of some chronic pain syndromes. Anesthesiology also evolved into a recognized medical specialty (as affirmed by the American Medical Association and the American Board of Medical Specialties), providing continuous improvement in patient care based on the introduction of new drugs and techniques made possible in large part by research in the basic and clinical sciences.
1. DEFINITION OF ANESTHESIOLOGY AS A SPECIALTY
A more formal definition of the specialty of anesthesiology is provided by The American Board of Anesthesiology (ABA). (1) The ABA defines anesthesiology as a discipline within the practice of medicine dealing with but not limited to:
- Assessment of, consultation for, and preparation of patients for anesthesia.
- Relief and prevention of pain during and following surgical, obstetric, therapeutic, and diagnostic procedures.
- Monitoring and maintenance of normal physiology during the perioperative period.
- Management of critically ill patients including those receiving their care in an intensive care unit.
- Diagnosis and treatment of acute, chronic, and cancer-related pain.
- Management of hospice and palliative care.
- Clinical management and teaching of cardiac, pulmonary, and neurologic resuscitation.
- Evaluation of respiratory function and application of respiratory therapy.
- Conduct of clinical, translational, and basic science research.
- Supervision, instruction, and evaluation of performance of both medical and allied health personnel involved in perioperative or periprocedural care, hospice and palliative care, critical care, and pain management.
- Administrative involvement in health care facilities and organizations, and medical schools as appropriate to the ABA’s mission.
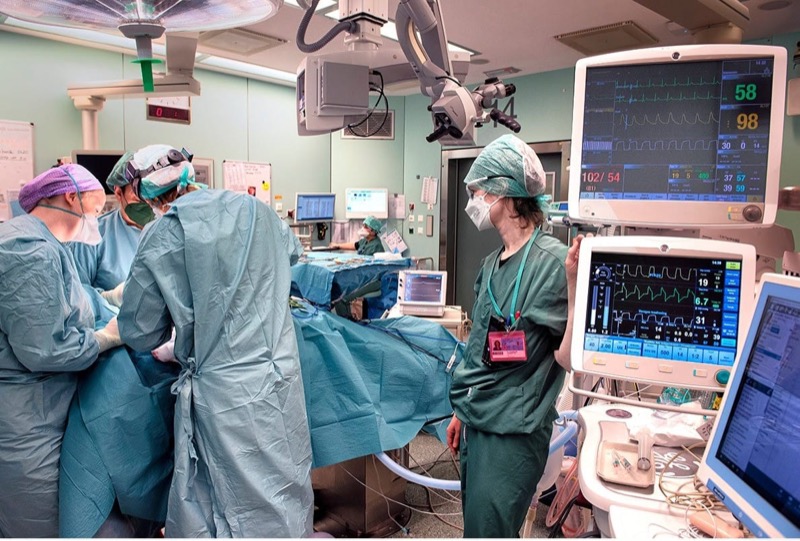
- Administration of anesthesia is often described as flying a plane. There is a take off (induction), in-flight (maintenance of anesthesia) and landing (emergence). Each of these three parts (there are many more) requires years of studying and practice for patient safety. An anesthesiologists must be vigilant, have a great focus, ability to multitask and the leadership skills for if (when) the crisis occurs to steer the entire OR team to the positive outcome.
As with other medical specialties, anesthesiology is represented by professional societies (American Society of Anesthesiologists, International Anesthesia Research Society), scientific journals (Anesthesiology, Anesthesia & Analgesia), a residency review committee with delegated authority from the Accreditation Council for Graduate Medical Education (ACGME) to establish and ensure compliance of anesthesia residency training programs with published standards, and a medical specialty board, the ABA, that establishes criteria for becoming a certified specialist in anesthesiology. The ABA, in conjunction with other specialty boards, has also developed criteria for maintenance of certification, which includes a program of continual self-assessment and lifelong learning, along with periodic assessment of professional standing, cognitive expertise in practice performance, and improvement. (1) This describes the American system. Other countries and societies have their systems to certify specialists in anesthesiology. Some countries work in a collective manner to educate and certify specialists in anesthesiology (e.g., European Society of Anesthesia).
2. EVOLUTION OF ANESTHESIA AS A MULTIDISCIPLINARY MEDICAL SPECIALTY
In the last 50 years, the medical specialty of anesthesiology has progressively extended its influence outside the operating rooms. Initially, the most important non–operating room patient care skills developed by anesthesia providers have been in pain management and adult critical care medicine. Beginning in the 1980s, anesthesia residency training required rotation experiences in these areas. In 1985, the ABA began issuing subspecialty certificates in critical care medicine to candidates who had completed at least a year of specialty training, thus becoming the first recognized subspecialty of anesthesiology. Pain medicine became the second subspecialty to be formally recognized when the ABA began issuing certificates in 1991. By this time, residency programs required rotations in multiple specialty areas, and fellowship programs in many areas were being developed. This reflected the progressive complexity of health care as well as extensive specialization in all fields of medicine.
Pain Management
Pain management is required in the perioperative setting as well as for chronic pain conditions. The management of perioperative pain has become more complex as the relationship between postoperative pain control and functional outcomes (e.g., mobility after joint replacement surgery) has become more tightly linked. In addition, the increasing use of neuraxial and regional anesthesia techniques for postoperative pain management has led to increasingly specialized acute pain management services usually managed by anesthesiology. An outpatient-based pain management center typically takes care of patients with chronic pain on an outpatient basis with occasional consultations in the hospital itself (e.g., for patients with chronic pain who require surgery that leads to acute and chronic pain). Many specialties are involved in chronic pain management, including neurology, neurosurgery, medicine, psychiatry, physical medicine, and physical therapy.
Critical Care Medicine
Critical care medicine has significantly increased in complexity over the 30 years it has been recognized as a distinct subspecialty of anesthesiology. Increasingly, data from large randomized clinical trials are used to develop patient care protocols. (2) The categorization of ICU patients is most often arranged by one or more specialties (e.g., medical, surgical, neurosurgical, cardiac). Because so many specialties can or need to be involved, the critical care medicine specialist may have his or her initial residency training in several different specialties, including anesthesiology, medicine, surgery, neurology, pulmonary medicine, nephrology, or emergency medicine. In many institutions, anesthesiologists are in local leadership roles in critical care medicine.
Pediatric Anesthesia
Since the 1980s, anesthesia residency training has included rotations in pediatric anesthesia (see Chapter 34), and separate pediatric anesthesia fellowships have been offered for many years. However, subspecialty certification by the ABA has only been issued since 2013. In 2009, the ABA and the American Board of Pediatrics launched a combined integrated training program in both pediatrics and anesthesiology that would take 5 years instead of the traditional 6 years. In pediatric hospitals, the role of pediatric anesthesiologists is very clear. However, the practice (and staffing challenges) becomes more complex when pediatric and adult surgeries are performed in the same hospital. Typical questions include how young must a patient be when only pediatric anesthesiologists deliver anesthesia (i.e., instead of anesthesiologists whose practice is mostly adult patients)? How should anesthesia be covered when there are no pediatric anesthesiologists? In a few hospitals, pediatric anesthesiologists also manage patients in the pediatric ICUs.
Cardiac Anesthesia
Cardiac anesthesia rotations have been required in residency for many years, and elective cardiac anesthesia fellowships have been available for at least as long. In 2006, the ACGME began to accredit adult cardiothoracic anesthesia fellowships, which led to increasing structure and standardization of the fellowships, including the requirement for echocardiography training. Anesthesiologists can obtain certification from the National Board of Echocardiography for perioperative transesophageal echocardiography as well as adult echocardiography. This certification is commonly achieved by cardiac anesthesiologists.
Obstetric Anesthesia
Because of the unique physiology and patient care issues, and the painful nature of childbirth, obstetric anesthesia experiences have always been an essential component of anesthesia training programs. Similarly, anesthesia fellowship training in obstetric anesthesia has been offered for decades. In 2012, the ACGME began to accredit obstetric anesthesiology fellowships. Similar to the evolution of other ACGME anesthesia fellowships (i.e., critical care, pain medicine, pediatric anesthesia, and adult cardiothoracic anesthesia), this has resulted in standardized and structured training to develop future leaders in obstetric anesthesia. Currently, the ABA does not offer subspecialty certification in this area.
Other Surgical Areas of Anesthesia
Anesthesia for the remaining surgical specialties is not associated with another certification process, although non-ACGME fellowship training may be available. These subspecialties include cardiothoracic, colon and rectal, general surgery, neurological, ophthalmic, oral and maxillofacial, urology, vascular, as well as hospice and palliative. Anesthesia for the remaining surgical subspecialties is frequently delivered by anesthesiologists without additional special training other than that provided by a standard anesthesiology residency. Often, institutional patient volume dictates whether specialized anesthesia teams can deliver anesthesia. For example, institutions with large outpatient or neurosurgical surgery may have separate specialized teams.
3. PERIOPERATIVE PATIENT CARE
Preoperative Evaluation
Perioperative care includes preoperative evaluation, preparation in the immediate preoperative period, intraoperative care, PACU, acute postoperative pain management, and possibly ICU care. Beginning in the late 1990s to early 2000s, most surgical patients were required to arrive the morning of surgery rather than the night before. This change frequently dictated that the anesthesia preoperative evaluation be performed during the morning of surgery. However, with complex patient medical risks and surgical procedures, many institutions created a preoperative clinic that allowed patients to be evaluated one or more days before the day of surgery. These clinics have become quite sophisticated and are often managed by anesthesiologists. Patients may be evaluated directly by anesthesiologists, or the anesthesiologist may oversee care provided by nurses or nurse practitioners. Periodically, a patient will need additional evaluation by the primary care physician or other specialists for specific patient care issues.
Operating Room Theaters
Operating room theaters are increasingly becoming management challenges (see Chapter 46). Matching operating room available time with predicted surgical complexity and length is an intellectual challenge in its own right. (1-4) “Throughput” is the term used to describe the efficiency of each patient’s experience. For decades, surgical teams have been allowed to operate in two to three operating rooms at the same time. For the first time in decades, the risks of concurrent surgeries are being questioned. (5) Sometimes the throughput is delayed not because of the operating room availability but because of insufficient beds in the PACU. There are numerous steps in the perioperative pathway (e.g., preoperative evaluation, the accuracy of predicting length and complexity of surgical care, and patient flow in and out of PACUs) that can delay a patient’s progress as scheduled. For example, patients may need to wait in the operating room when surgery is complete awaiting a bed in the PACU. Institutions are increasingly appointing perioperative or operating room directors who either manage the operating rooms or coordinate the entire perioperative process starting from the preoperative clinic until exit from the PACU. These positions can be administratively challenging and require considerable skill and clinical savvy. Such jobs are frequently held by an anesthesiologist, although sometimes the director might be a surgeon, nurse, or hospital administrator.
Postanesthesia Care Unit
In a tertiary care hospital, the role of the PACU is pivotal. Not only are patients recovering from anesthesia and surgery, they also are receiving direction for appropriate care after their PACU time that spans from ICU to discharge. Even now, insufficient PACU beds are often a cause of delayed throughput in operating room theaters.(1-4) There are many scenarios that illustrate this basic problem. If the routine hospital beds are completely occupied, there is no place to transfer fully recovered patients in the PACU. If those patients stay in the PACU, there will then be no beds for patients who need recovery from operating room–based surgery and anesthesia. When this problem is anticipated, then surgery start times are delayed. In the future, as anesthesiologists take care of patients with more complex medical risks, more PACU beds will be required in hospitals. In addition to the quality of care, patient logistical management is key to the quality and efficiency of care in the perioperative period.
4. TRAINING AND CERTIFICATION IN ANESTHESIOLOGY
Postgraduate (Residency) Training in Anesthesiology
Postgraduate training in anesthesiology in the United States consists of 4 years of supervised experience in an approved program after the degree of doctor of medicine or doctor of osteopathy has been obtained. The first year of postgraduate training in anesthesiology consists of education in the fundamental clinical skills of medicine. The second, third, and fourth postgraduate years (clinical anesthesia years 1 to 3) are spent learning all aspects of clinical anesthesia, including subspecialty experience in obstetric anesthesia, pediatric anesthesia, cardiothoracic anesthesia, neuroanesthesia, anesthesia for outpatient surgery, recovery room care, regional anesthesia, and pain management. In addition to these subspecialty experiences, 4 months of training in critical care medicine is required. The duration and structure of anesthesiology education differ in countries around the world. Nevertheless, there is generalized international agreement on what constitutes adequate training in anesthesiology and its perioperative responsibilities.
The content of the educational experience during the clinical anesthesia years reflects the wide-ranging scope of anesthesiology as a medical specialty. Indeed, the anesthesiologist should function as the clinical pharmacologist and internist or pediatrician in the operating room. Furthermore, the scope of anesthesiology extends beyond the operating room to include acute and chronic pain management, critical care medicine, cardiopulmonary resuscitation, and research. More recently, anesthesia training programs have been given increasingly more flexibility. Programs can offer integrated residency and fellowship training, including options for significant research time. These more specialized training programs have the opportunity to produce leaders in subspecialty clinical areas and research. In addition, the ABA has supported the development of combined residency programs in anesthesia and internal medicine, anesthesia and pediatrics, and, most recently, anesthesia and emergency medicine. Clearly, anesthesia training programs are being encouraged to train anesthesiologists who can meet the challenges of the future.
Approximately 131 postgraduate training programs in anesthesiology are approved by the ACGME in the United States. Approved programs are reviewed annually by the Residency Review Committee (RRC) for Anesthesiology to ensure continued compliance with the published program requirements. The RRC for Anesthesiology consists of members appointed by the American Medical Association, the American Society of Anesthesiologists, and the ABA.
American Board of Anesthesiology
The ABA was incorporated as an affiliate of the American Board of Surgery in 1938. After the first voluntary examination, 87 physicians were certified as diplomates of the ABA. The ABA was recognized as an independent board by the American Board of Medical Specialties in 1941. To date, more than 30,000 anesthesiologists have been certified as diplomates of the ABA based on completing an accredited postgraduate training program, passing a written and oral examination, and meeting licensure and credentialing requirements. These diplomates are referred to as “board-certified anesthesiologists,” and the certificate granted by the ABA is characterized as the primary certificate. Starting on January 1, 2000, the ABA, like most other specialty boards, began to issue time-limited certificates (10-year limit). To recertify, all diplomates must participate in a program designated Maintenance of Certification in Anesthesiology (MOCA). In 2016, this program was newly redesigned as MOCA 2.0. Diplomates whose certificates are not time limited (any certificate issued before January 1, 2000) may participate voluntarily in MOCA. The MOCA program emphasizes continuous self-improvement (cornerstone of professional excellence) and evaluation of clinical skills and practice performance to ensure quality, as well as public accountability. The components include (1) professionalism and professional standing (unrestricted state license), (2) lifelong learning and self-assessment (formal and informal continuing medical education [CME], including patient safety), (3) assessment of knowledge, judgment, and skills (completing 30 MOCA minute pilot questions per calendar quarter), and (4) improvement in medical practice. This final component may include a variety of self-directed activities including simulation, quality improvement projects, or clinical pathway development.6 Along with several other specialties, the ABA also issues certificates in pain medicine, critical care medicine, hospice and palliative medicine, sleep medicine, and pediatric anesthesiology to diplomates who complete 1 year of additional postgraduate training in the respective subspecialty, meet licensure and credentialing requirements, and pass a written examination. These certificates also have a 10-year time limit. Recertification requirements are continuing to evolve as part of the ABA transition to Maintenance of Certification in Anesthesiology for Subspecialties Program (MOCA-SUBS).
Credentialing and Privileging
After completing residency and joining the medical staff of a hospital, the anesthesiologist must undergo the credentialing and privileging process, which allows appropriate institutions to collect, verify, and evaluate all data regarding a clinician’s professional performance. Recently, three new concepts were developed on a joint basis by the ACGME and the American Board of Medical Specialties. General competencies (i.e., patient care, medical/clinical knowledge, practiced-based learning and improvement, interpersonal and communication skills, professionalism, and systems-based practice) are used by the medical staff to evaluate clinicians. Also, focused professional practice evaluation can be used to provide more thorough information about an individual clinician. The last new concept is ongoing professional practice evaluation. In essence, processes need to be developed to identify a problem as soon as possible.
5. OTHER ANESTHETIC PROVIDERS
Certified Registered Nurse Anesthetists
Certified registered nurse anesthetists (CRNAs) probably participate in more than 50% of the anesthetics administered in the United States, most often under the supervision of a physician. To become a CRNA, the candidate must earn a registered nurse degree, spend 1 year as a critical care nurse, and then complete 2 to 3 years of didactic and clinical training in the techniques of administration of anesthetics in an approved nurse anesthesia training program. The American Association of Nurse Anesthetists is responsible for the curriculum of nurse anesthesia training programs, as well as the establishment of criteria for certification as a CRNA. The activities of CRNAs frequently concern the intraoperative care of patients during anesthesia while working under the supervision (medical direction) of an anesthesiologist. This physician-nurse anesthetist team approach (anesthesia care team) is consistent with the concept that administration of anesthesia is the practice of medicine. In some situations CRNAs administer anesthesia without the supervision or medical direction of an anesthesiologist.
Anesthesiologist Assistants
Anesthesiologist assistants complete a graduate-level program (about 27 months) and receive a master of medical science in anesthesia from an accredited training program (currently Case Western Reserve University, Emory University School of Medicine, Nova Southeastern University, South University, and University of Missouri). (3,7) Anesthesiologist assistants work cooperatively under the direction of the anesthesiologist as members of the anesthesia care team to implement the anesthesia care plan.
6. QUALITY OF CARE AND SAFETY IN ANESTHESIA
Continuous Quality Improvement
Quality is a difficult concept to define in the practice of medicine. It is generally agreed, however, that attention to quality improves patient safety and satisfaction with anesthetic care. Although the specialty of anesthesiology has had such emphasis for a long time, the National Academies of Sciences, Engineering, and Medicine (formerly the Institute of Medicine) drew attention to these issues in medicine overall in 2000 with their report “To Err Is Human.” (4,8) New frequently used words became a routine part of our vocabulary (e.g., metrics of competency, ongoing measurement, standardization, checklists, timeouts, system approaches, and practice parameters). (5,6,9,10) Quality improvement programs in anesthesia are often guided by requirements of The Joint Commission (formerly the Joint Commission on Accreditation of Healthcare Organizations [JCAHO]). Quality of care is evaluated by attention to (1) structure (personnel and facilities used to provide care), (2) process (sequence and coordination of patient care activities such as performance and documentation of a preanesthetic evaluation, and continuous attendance to and monitoring of the patient during anesthesia), and (3) outcome. A quality improvement program focuses on measuring and improving these three basic components of care. In contrast to quality assurance programs designed to identify “outliers,” continuous quality improvement (CQI) programs take a “systems” approach in recognition of the fact that random errors are inherently difficult to prevent. System errors, however, should be controllable and strategies to minimize them should be attainable. A CQI program may focus on undesirable outcomes as a way to identify opportunities for improvement in the structure and process of care.
Improvement in quality of care is often measured by a decrease in the rate of adverse outcomes. However, the relative rarity of adverse outcomes in anesthesia makes measurement of improvement difficult. To complement outcome measurement, CQI programs may focus on critical incidents and sentinel events. Critical incidents (e.g., ventilator disconnection) are events that cause or have the potential to cause injury if not noticed and corrected in a timely manner. Measurement of the occurrence rate of important critical incidents may serve as a substitute for rare outcomes in anesthesia and lead to improvement in patient safety. Sentinel events are isolated events that may indicate a systematic problem (syringe swap because of poor labeling, drug administration error related to keeping unneeded medications on the anesthetic cart).
The key factors in the prevention of patient injury related to anesthesia are vigilance, up-to-date knowledge, and adequate monitoring. Obviously, it is important to follow the standards endorsed by the American Society of Anesthesiologists. In this regard, American anesthesiology has been a leader within organized medicine in the development and implementation of formal, published standards of practice. These standards have significantly influenced how anesthesia is practiced in the United States (e.g., practice parameters). (6,10)
The publicity and emphasis on quality and safety have been intense for several years, but sometimes the standards are not implemented as rapidly and completely as desired. Recently suggestions have been made to attach credentialing requirements and penalties for failure to adhere to the required practices. (7,11)
7. ORGANIZATIONS WITH EMPHASIS ON ANESTHESIA QUALITY AND SAFETY
Anesthesia Patient Safety Foundation
The Anesthesia Patient Safety Foundation (APSF) was established under the administration of Ellison C. Pierce, Jr., MD, during his year as president of the American Society of Anesthesiologists. (8,12) Initial financial support for formation of the APSF was provided by the American Society of Anesthesiologists, and this financial support continues to the present. In addition, APSF receives financial support from corporations, specialty societies, and individual donors. The purpose of APSF is to “assure that no patient shall be harmed by anesthesia.” To fulfill this mission, the APSF provides research grants to support investigations designed to provide a better understanding of preventable anesthetic injuries and promotes national and international communication of information and ideas about the causes and prevention of harm from anesthesia. A quarterly APSF newsletter is the most widely distributed anesthesia publication in the world and is dedicated to discussion of anesthesia patient safety issues. Anesthesiology is the only specialty in medicine with a foundation dedicated solely to issues of patient safety. The National Patient Safety Foundation, formed in 1997 by the American Medical Association, is modeled after the APSF.
Anesthesia Quality Institute
The Anesthesia Quality Institute (AQI) was formed in 2008 for the purpose of being a primary source of information for quality improvement in the practice of anesthesiology. It maintains data that can be used to “assess and improve patient care.” Eventually, the AQI will be able to provide quality and safety data that could be used to meet regulatory requirements. The AQI is already being used as a source of data for clinical care, research, and societies that have improving quality of care as a goal. The AQI website describes the structure of the National Anesthesia Clinical Outcomes Registry (NACOR) and how data flow into and out of the AQI. (13)
American Society of Anesthesiologists Closed Claims Project and Its Registries
The ASA Closed Claims Project and its Registries are a database of retrospective analyses of legal cases with adverse outcomes. This ongoing investigation has helped identify patient and practice risk areas that tend to have difficulties and require added attention from the specialty with regard to quality and safety. (5,9)
Foundation for Anesthesia Education and Research
Although not directly involved with quality and safety, the Foundation for Anesthesia Education and Research (FAER) is an exceptionally important vehicle for support of research in the specialty of anesthesiology. FAER was established in 1986 with financial support from the American Society of Anesthesiologists. In addition, FAER receives financial support from corporations, specialty societies, and individual donors. The purpose of FAER is to encourage research, education, and scientific innovation in anesthesiology, perioperative medicine, and pain management. Over the years, FAER has funded numerous research grants and provided support for the development of academic anesthesiologists.
8. PROFESSIONAL LIABILITY
Because of intense dedication to quality and safety, malpractice claims have been reduced both in frequency and magnitude. As a result, malpractice premiums have dramatically decreased over the last 20 years. Nevertheless the fundamental principles need to be understood. First, litigation still occurs. For example, 93 claims were filed in the United Kingdom over the years 1995 to 2007. (9,14) Sixty-two claims involved alleged drug administration errors in which muscle relaxants were the most common issue. Also, 19 claims involved patients being awake and paralyzed. With proper labeling and double-checking, such errors can be decreased. The anesthesiologist is clearly responsible for management and recovery from anesthesia. Physicians administering anesthetics are not expected to guarantee a favorable outcome to the patient but are required to exercise ordinary and reasonable care or skill in comparison to other anesthesiologists. That the anticipated result does not follow or that complications occur does not imply negligence (practice below the standard of care). Furthermore, an anesthesiologist is not responsible for an error in judgment unless it is viewed as inconsistent with the skill expected of every physician. As a specialist, however, an anesthesiologist is responsible for making medical judgments that are consistent with national, not local, standards. Anesthesiologists maintain professional liability (malpractice) insurance that provides financial protection in the event of a court judgment against them. Also, CRNAs can be held legally responsible for the technical aspects of the administration of anesthesia. It is likely, however, that legal responsibility for the actions of the CRNA will be shared by the physician responsible for supervising the administration of anesthesia.
The best protection for the anesthesiologist against medicolegal action lies in the thorough and up-to-date practice of anesthesia, coupled with interest in the patient by virtue of preoperative and postoperative visits plus detailed records of the course of anesthesia (automated information systems provide the resource to collect and record real-time actual data). Also, all anesthesia providers should be prepared to transition to anesthesia record keeping via automated information systems. Specifically, use of automated anesthetic records should be fully integrated into one’s medical center information technology system. Unfortunately, implementation of electronic health records (EHRs) is difficult, costly, time-consuming, and fraught with many unintended consequences, including not meeting safety standards. However, a review of 2008-2014 national data reveals large gains in using EHRs with 75% of hospitals having at least a basic EHR system, up from 59% in 2013. (15) In the United States, at the forefront of implementation and use of health information technology is the Office of the National Coordinator (ONC) for Health Information Technology.
Adverse Events
In the event of an accident or complication related to the administration of anesthesia, the anesthesiologist should promptly document the facts on the patient’s medical record and immediately notify the appropriate agencies, beginning at the department level and continuing with one’s own medical center quality improvement administration and risk management office. Patient treatment should be noted and consultation with other physicians sought when appropriate. The anesthesiologist should provide the hospital and the company that writes the physician’s professional liability insurance with a complete account of the incident. The investigation and discussion of adverse events and complications may involve a root cause analysis (RCA) in collaboration with the physicians, nurses, and other staff involved with the patient’s care.
9. RISKS OF ANESTHESIA
Although patients may express a fear of dying during anesthesia, the fact is that anesthesia-related deaths have decreased dramatically in the last 2 decades. (11,17) Because fewer adverse events are being attributed to anesthesia, the professional liability insurance premiums paid by anesthesiologists have decreased. (12,18) The increased safety of anesthesia (especially for patients without significant coexisting diseases and undergoing elective surgery) is presumed to reflect the introduction of improved anesthesia drugs and monitoring (pulse oximetry, capnography), as well as the training of increased numbers of anesthesiologists. Despite the perceived safety of anesthesia, adverse events still occur, and not all agree that the mortality rate from anesthesia has improved as greatly as suggested. Improvement is based on a series of 244,000 surviving patients who underwent anesthesia and surgery. This series is the basis for estimating a mortality rate from anesthesia of 1 in 250,000. (14,19) It is likely that the safety of anesthesia and surgery can be improved by persuading patients to stop smoking, lose weight, avoid excess intake of alcohol, and achieve optimal medical control of essential hypertension, diabetes mellitus, and asthma before undergoing elective operations.
When perioperative adverse events occur, it is often difficult to establish a cause-and-effect mechanism. In many instances it is impossible to separate an adverse event caused by an inappropriate action of the anesthesiologist (“lapse of vigilance,” breach in the standard of care) from an unavoidable mishap (maloccurrence, coincidental event) that occurred despite optimal care. (15,20) Examples of adverse outcomes other than death include peripheral nerve damage, brain damage, airway trauma (most often caused by difficult tracheal intubation), intraoperative awareness, eye injury, fetal/newborn injury, and aspiration. Difficult airway management has traditionally been perceived by anesthesiologists as the greatest anesthesia patient safety issue. (17,21) A survey of large anesthesia groups has highlighted other concerns to patient safety.
Improved monitoring of anesthetized patients hopefully will serve to further enhance the vigilance of the anesthesiologist and decrease the role of human error in anesthetic morbidity and mortality rates. Indeed, human error, in part resulting from lapses in attention (vigilance), accounts for a large proportion of adverse anesthesia events. A number of factors at work in the operating room environment serve to diminish the ability of the anesthesiologist to perform the task of vigilance. Prominent among these factors are sleep loss and fatigue with known detrimental effects on work efficiency and cognitive tasks (monitoring, clinical decision making). The RRC for Anesthesiology mandates that anesthesia residents not be assigned clinical responsibilities the day after 24-hour in-hospital call. The Health and Medicine Division (HMD) of the National Academies has made very specific recommendations regarding resident work hours and will no doubt make recommendations for physicians overall that could eventually be mandated. The emphasis on efficiency in the operating room (“production pressures”) designed to improve productivity may supersede safety and provoke the commission of errors that jeopardize patient safety. At the same time, not all adverse events during anesthesia are a result of human error and therefore preventable
10. HAZARDS OF WORKING IN THE OPERATING ROOM
Anesthesiologists spend long hours in an environment (operating room) associated with exposure to vapors from chemicals (volatile anesthetics), ionizing radiation, and infectious agents (hepatitis viruses, human immunodeficiency virus). There is psychological stress from demands of the constant vigilance required for the care of patients during anesthesia. Furthermore, interactions with members of the operating team (surgeons, nurses) may introduce varying levels of interpersonal stress. Removal of waste anesthetic gases (scavenging) has decreased exposure to trace concentrations of these gases, although evidence that this practice has improved the health of anesthesia personnel is lacking. Universal precautions are recommended in the care of every patient in an attempt to prevent the transmission of blood-borne infections, particularly by accidental needlestick injuries. Substance abuse, mental illness (depression), and suicide seem to occur with increased frequency among anesthesiologists, perhaps reflecting the impact of occupational stress.
Lastly, infection control for both patients and clinical personnel in the operating rooms require increasingly strict rules regarding specific procedures in the operating room such as washing hands.
11. SUMMARY AND FUTURE OUTLOOK
This chapter reflects the constantly evolving and changing practice of anesthesia. Our responsibilities have grown in magnitude, scope, and depth. Although anesthesia practice is partly based on outpatient activities, it has also become a leading specialty with regard to inpatient medicine, especially the perioperative period including critical care medicine. Definitely more sophisticated technological tools and systems will be integrated in the practice of anesthesiology. In more recent years, the use of robots in the operating theater has become standard for specific surgeries. (18,22) The specialty will become even more valuable to medicine overall by attempting to anticipate future societal needs (15,20) and continuing to dedicate ourselves to the pursuit of excellence. (10) Lastly, this chapter has described the American organization and delivery of anesthesia. Every country in the world has or should subject their anesthesia practice to an intense and possibly similar type of analysis.
12. QUESTIONS OF THE DAY
- In the United States, which anesthesiology fellowships are accredited by the Accreditation Council for Graduate Medical Education? What is the impact of Accreditation Council for Graduate Medical Education accreditation on the structure of a fellowship program?
- What are the sources of data in the National Anesthesia Clinical Outcomes Registry?
- How has the Foundation for Anesthesia Education and Research helped to advance the specialty of anesthesiology?
- What are the reasons for a decrease in anesthesia malpractice premiums over the past few decades? What steps can the anesthesia provider take to reduce the chance for a lawsuit after an adverse event?
- What are the potential hazards of working in the operating room as an anesthesia provider?