Dexmedetomidine in Carotid Surgery: Less Propofol, Better Stability?
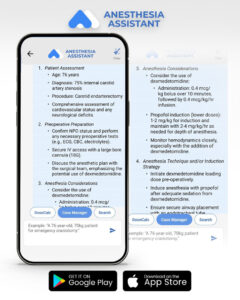
A new randomized controlled trial by Vetter et al. published in the European Journal of Anaesthesiology (2025) sheds light on the significant benefits of combining dexmedetomidine with total intravenous anesthesia (TIVA) in patients undergoing carotid endarterectomy (CEA). Conducted at the University Hospital of Bern, Switzerland, this single-center trial demonstrates that dexmedetomidine not only reduces propofol requirements but also improves hemodynamic stability without compromising neurophysiological monitoring or recovery.
Key findings at a glance
- Reduction in Propofol requirements: Dexmedetomidine lowered the propofol effect-site concentration required for burst suppression by 33%.
- Improved hemodynamic stability: Patients receiving dexmedetomidine required 50% less norepinephrine to maintain target blood pressures.
- Preservation of neurophysiology: No significant adverse effects on intraoperative somatosensory (SEP) or motor-evoked potentials (MEP).
- No increase in postoperative delirium: Cognitive recovery and delirium rates were comparable between groups.
Background: Why Dexmedetomidine?
CEA is a surgical procedure to reduce the risk of stroke in patients with internal carotid artery (ICA) stenosis. General anesthesia (GA), particularly TIVA with propofol, is often preferred to facilitate intraoperative neurophysiological monitoring (IONM).
However, inducing burst suppression (BS) with propofol to lower cerebral metabolic demand often requires high doses, resulting in:
- Increased vasopressor needs
- Hemodynamic fluctuations
- Delayed emergence
Dexmedetomidine, an alpha-2 adrenergic agonist, has shown promise for:
- Reducing anesthetic requirements
- Stabilizing blood pressure
- Offering potential neuroprotective effects
Study design and methods
Inclusion criteria:
- ASA physical status ≤ 4
- Symptomatic/asymptomatic ICA stenosis
- Age ≥ 18 years
Exclusion criteria:
- Significant cardiac arrhythmias, bradycardia, severe hypovolemia
- Liver disease, known propofol/dexmedetomidine hypersensitivity
- Pregnancy, cardiovascular instability, limited autonomic activity
Dexmedetomidine group:
- Bolus: 0.4 µg/kg over 10 minutes before induction
- Infusion: 0.4 µg/kg/h until surgical closure
Control group:
- Standard TIVA without dexmedetomidine
Both groups:
- Propofol administered via target-controlled infusion (TCI)
- Titrated to achieve EEG burst suppression (verified via raw EEG and spectral analysis)
- Remifentanil and fentanyl for analgesia
- Normoventilation maintained
Primary outcome
Effect-site concentration of Propofol during burst Suppression
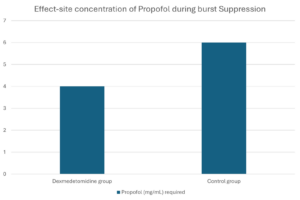
Result: Significant reduction
Secondary outcomes
Vasoactive drug requirement
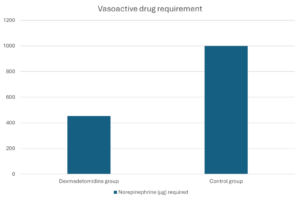
Result: 50% reduction in vasopressor need
Neurophysiological monitoring
- SEP and MEP remained stable
- Minor non-significant changes in MEP thresholds observed post-BS
- No interference with detection of ischemic changes
Postoperative assessment
- Delirium: Assessed via CAM-ICU score on postoperative day one
- No significant differences were observed between the groups
- GCS scores were consistently favorable (15 in most patients)
- No delayed emergence from anesthesia
Discussion: Clinical implications
- Propofol-sparing effect: Reduced propofol dosage minimizes cardiovascular depression and speeds recovery.
- Improved Haemodynamics: Dexmedetomidine’s alpha-2 agonism maintains mean arterial pressure (MAP) closer to baseline. Avoids swings in blood pressure, which is key in preventing hyperperfusion syndrome.
- Neurophysiology integrity: Unlike concerns raised in earlier studies, dexmedetomidine did not impair intraoperative SEP/MEP monitoring.
- Delirium and cognitive recovery: While the trial was not specifically powered to evaluate long-term cognitive outcomes, the incidence of delirium was notably low.
Step-by-step protocol summary
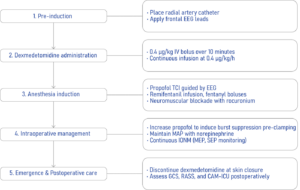
This study provides robust evidence supporting the co-administration of dexmedetomidine with TIVA during carotid endarterectomy:
- Reduces propofol and vasopressor needs
- Maintains neurophysiological integrity
- Enhances hemodynamic stability
These findings have direct clinical relevance, suggesting that integrating dexmedetomidine into CEA protocols may improve intraoperative and immediate postoperative outcomes.
Reference: Vetter C, Meyer ER, Seidel K, Bervini D, Huber M, Krejci V. Co-administration of dexmedetomidine with total intravenous anaesthesia in carotid endarterectomy reduces requirements for propofol and improves haemodynamic stability: A single-centre, prospective, randomised controlled trial. Eur J Anaesthesiol. 2025;42(3):255-264.
For more information on Dexmedetomidine, check out Anesthesia Updates on the NYSORA Anesthesia Assistant App.
Get access to step-by-step management algorithms, the latest research, and peer-reviewed insights—all in one place. Download the app today and experience the future of anesthesia education and decision-making.